Aims: To introduce a case report and review the literature on trauma-related acute macular neuroretinopathy as an unusual etiology of acute macular neuroretinopathy.
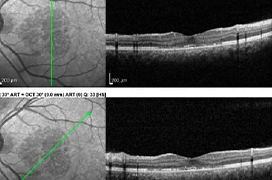
Material and Methods: A 24-year-old man presented with unilateral paracentral scotoma following non-ocular trauma in a car accident. The relative afferent pupillary defect was negative and the best corrected visual acuities of both eyes were 10/10 (by the Snellen chart scale). Results: Retinoscopy revealed a reduced foveal reflex, along with a small pre-retinal hemorrhage over the mid-pathway of the supranasal arteriole. OCT images showed an obvious ellipsoid zone (EZ) layer disruption in the macula of the left eye. The infrared fundus photograph of the same eye revealed a distinct hyporeflective area involving the macula. On fundus angiography, no macular vascular lesion was detected. The scotoma persisted after 3 months follow-up.
Conclusion: Non-ocular trauma including head or chest trauma without direct ocular injury accounts for most cases of trauma-related acute macular neuroretinopathy. It is important to distinguish this entity, given that there are also unremarkable findings in the retinal examination of these patients. Indeed, proper clinical suspicion leads to further suitable investigations and impedes other extraordinary images, which are the basic rules in the management of traumatic patients suffering multiple injuries and incurring medical expenses.